InVivoPlus anti-mouse CTLA-4 (CD152)
Product Description
Specifications
| Isotype | Mouse IgG2b |
|---|---|
| Recommended Isotype Control(s) | InVivoPlus mouse IgG2b isotype control, unknown specificity |
| Recommended Dilution Buffer | InVivoPure pH 7.0 Dilution Buffer |
| Conjugation | This product is unconjugated. Conjugation is available via our Antibody Conjugation Services. |
| Immunogen | Not available or unknown |
| Reported Applications |
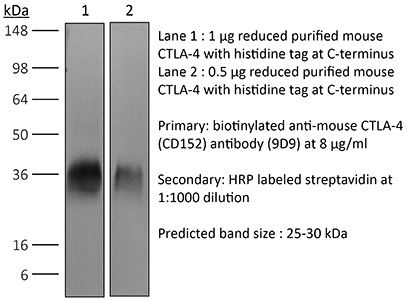
in vivo CTLA-4 neutralization Western blot in vivo intra-tumoral regulatory T cell depletion in vitro Organoids/Organ-on-Chip |
| Formulation |
PBS, pH 7.0 Contains no stabilizers or preservatives |
| Endotoxin* |
≤0.5EU/mg (≤0.0005EU/μg) Determined by LAL assay |
| Aggregation* |
<5% Determined by SEC |
| Purity |
≥95% Determined by SDS-PAGE |
| Sterility | 0.2 µm filtration |
| Production | Purified from cell culture supernatant in an animal-free facility |
| Purification | Protein A |
| RRID | AB_10949609 |
| Molecular Weight | 150 kDa |
| Murine Pathogen Tests* |
Ectromelia/Mousepox Virus: Negative Hantavirus: Negative K Virus: Negative Lactate Dehydrogenase-Elevating Virus: Negative Lymphocytic Choriomeningitis virus: Negative Mouse Adenovirus: Negative Mouse Cytomegalovirus: Negative Mouse Hepatitis Virus: Negative Mouse Minute Virus: Negative Mouse Norovirus: Negative Mouse Parvovirus: Negative Mouse Rotavirus: Negative Mycoplasma Pulmonis: Negative Pneumonia Virus of Mice: Negative Polyoma Virus: Negative Reovirus Screen: Negative Sendai Virus: Negative Theiler’s Murine Encephalomyelitis: Negative |
| Storage | The antibody solution should be stored at the stock concentration at 4°C. Do not freeze. |
| Need a Custom Formulation? | See All Antibody Customization Options |
Application References
-
Redmond, W. L., et al (2014). "Combined targeting of costimulatory (OX40) and coinhibitory (CTLA-4) pathways elicits potent effector T cells capable of driving robust antitumor immunity" Cancer Immunol Res 2(2): 142-153.
PubMed
Ligation of the TNF receptor family costimulatory molecule OX40 (CD134) with an agonist anti-OX40 monoclonal antibody (mAb) enhances antitumor immunity by augmenting T-cell differentiation as well as turning off the suppressive activity of the FoxP3(+)CD4(+) regulatory T cells (Treg). In addition, antibody-mediated blockade of the checkpoint inhibitor CTLA-4 releases the “brakes” on T cells to augment tumor immunotherapy. However, monotherapy with these agents has limited therapeutic benefit particularly against poorly immunogenic murine tumors. Therefore, we examined whether the administration of agonist anti-OX40 therapy in the presence of CTLA-4 blockade would enhance tumor immunotherapy. Combined anti-OX40/anti-CTLA-4 immunotherapy significantly enhanced tumor regression and the survival of tumor-bearing hosts in a CD4 and CD8 T cell-dependent manner. Mechanistic studies revealed that the combination immunotherapy directed the expansion of effector T-bet(high)/Eomes(high) granzyme B(+) CD8 T cells. Dual immunotherapy also induced distinct populations of Th1 [interleukin (IL)-2, IFN-gamma], and, surprisingly, Th2 (IL-4, IL-5, and IL-13) CD4 T cells exhibiting increased T-bet and Gata-3 expression. Furthermore, IL-4 blockade inhibited the Th2 response, while maintaining the Th1 CD4 and effector CD8 T cells that enhanced tumor-free survival. These data demonstrate that refining the global T-cell response during combination immunotherapy can further enhance the therapeutic efficacy of these agents.
-
Dai, M., et al (2015). "Curing mice with large tumors by locally delivering combinations of immunomodulatory antibodies" Clin Cancer Res 21(5): 1127-1138.
PubMed
PURPOSE: Immunomodulatory mAbs can treat cancer, but cures are rare except for small tumors. Our objective was to explore whether the therapeutic window increases by combining mAbs with different modes of action and injecting them into tumors. EXPERIMENTAL DESIGN: Combinations of mAbs to CD137/PD-1/CTLA-4 or CD137/PD-1/CTLA-4/CD19 were administrated intratumorally to mice with syngeneic tumors (B16 and SW1 melanoma, TC1 lung carcinoma), including tumors with a mean surface of approximately 80 mm(2). Survival and tumor growth were assessed. Immunologic responses were evaluated using flow cytometry and qRT-PCR. RESULTS: More than 50% of tumor-bearing mice had complete regression and long-term survival after tumor injection with mAbs recognizing CD137/PD-1/CTLA-4/CD19 with similar responses in three models. Intratumoral injection was more efficacious than intraperitoneal injection in causing rejection also of untreated tumors in the same mice. The three-mAb combination could also induce regression, but was less efficacious. There were few side effects, and therapy-resistant tumors were not observed. Transplanted tumor cells rapidly caused a Th2 response with increased CD19 cells. Successful therapy shifted this response to the Th1 phenotype with decreased CD19 cells and increased numbers of long-term memory CD8 effector cells and T cells making IFNgamma and TNFalpha. CONCLUSIONS: Intratumoral injection of mAbs recognizing CD137/PD-1/CTLA-4/CD19 can eradicate established tumors and reverse a Th2 response with tumor-associated CD19 cells to Th1 immunity, whereas a combination lacking anti-CD19 is less effective. There are several human cancers for which a similar approach may provide clinical benefit.
-
Dai, M., et al (2013). "Long-lasting complete regression of established mouse tumors by counteracting Th2 inflammation" J Immunother 36(4): 248-257.
PubMed
40% of mice with SW1 tumors remained healthy >150 days after last treatment and are probably cured. Therapeutic efficacy was associated with a systemic immune response with memory and antigen specificity, required CD4 cells and involved CD8 cells and NK cells to a less extent. The 3 mAb combination significantly decreased CD19 cells at tumor sites, increased IFN-gamma and TNF-alpha producing CD4 and CD8 T cells and mature CD86 dendritic cells (DC), and it increased the ratios of effector CD4 and CD8 T cells to CD4Foxp3 regulatory T (Treg) cells and to CD11bGr-1 myeloid suppressor cells (MDSC). This is consistent with shifting the tumor microenvironment from an immunosuppressive Th2 to an immunostimulatory Th1 type and is further supported by PCR data. Adding an anti-CD19 mAb to the 3 mAb combination in the SW1 model further increased therapeutic efficacy. Data from ongoing experiments show that intratumoral injection of a combination of mAbs to CD137PD-1CTLA4CD19 can induce complete regression and dramatically prolong survival also in the TC1 carcinoma and B16 melanoma models, suggesting that the approach has general validity.”}” data-sheets-userformat=”{“2″:14851,”3”:{“1″:0},”4”:{“1″:2,”2″:16777215},”12″:0,”14”:{“1″:2,”2″:1521491},”15″:”Roboto, sans-serif”,”16″:12}”>Mice with intraperitoneal ID8 ovarian carcinoma or subcutaneous SW1 melanoma were injected with monoclonal antibodies (mAbs) to CD137PD-1CTLA4 7-15 days after tumor initiation. Survival of mice with ID8 tumors tripled and >40% of mice with SW1 tumors remained healthy >150 days after last treatment and are probably cured. Therapeutic efficacy was associated with a systemic immune response with memory and antigen specificity, required CD4 cells and involved CD8 cells and NK cells to a less extent. The 3 mAb combination significantly decreased CD19 cells at tumor sites, increased IFN-gamma and TNF-alpha producing CD4 and CD8 T cells and mature CD86 dendritic cells (DC), and it increased the ratios of effector CD4 and CD8 T cells to CD4Foxp3 regulatory T (Treg) cells and to CD11bGr-1 myeloid suppressor cells (MDSC). This is consistent with shifting the tumor microenvironment from an immunosuppressive Th2 to an immunostimulatory Th1 type and is further supported by PCR data. Adding an anti-CD19 mAb to the 3 mAb combination in the SW1 model further increased therapeutic efficacy. Data from ongoing experiments show that intratumoral injection of a combination of mAbs to CD137PD-1CTLA4CD19 can induce complete regression and dramatically prolong survival also in the TC1 carcinoma and B16 melanoma models, suggesting that the approach has general validity.
-
Wei, H., et al (2013). "Combinatorial PD-1 blockade and CD137 activation has therapeutic efficacy in murine cancer models and synergizes with cisplatin" PLoS One 8(12): e84927.
PubMed
90 days (and was probably curative) by a mechanism which included a systemic CD8(+) T cell response with tumor specificity and immunological memory. Strikingly, combined treatment of cisplatin and CD137/PD-1 mAb also gave rise to the long-term survival of mice with established TC1 lung tumors. A similar combination of the 2 mAbs and cisplatin should be considered for clinical ‘translation’.”}” data-sheets-userformat=”{“2″:14851,”3”:{“1″:0},”4”:{“1″:2,”2″:16777215},”12″:0,”14”:{“1″:2,”2″:1521491},”15″:”Roboto, sans-serif”,”16″:12}”>There is an urgent need for improved therapy for advanced ovarian carcinoma, which may be met by administering immune-modulatory monoclonal antibodies (mAbs) to generate a tumor-destructive immune response. Using the ID8 mouse ovarian cancer model, we investigated the therapeutic efficacy of various mAb combinations in mice with intraperitoneal (i.p.) tumor established by transplanting 3 x 10(6) ID8 cells 10 days previously. While most of the tested mAbs were ineffective when given individually or together, the data confirm our previous finding that 2 i.p. injections of a combination of anti-CD137 with anti-PD-1 mAbs doubles overall survival. Mice treated with this mAb combination have a significantly increased frequency and total number of CD8(+) T cells both in the peritoneal lavage and spleens, and these cells are functional as demonstrated by antigen-specific cytolytic activity and IFN-gamma production. While administration of anti-CD137 mAb as a single agent similarly increases CD8(+) T cells, these have no functional activity, which may be attributed to up-regulation of co-inhibitory PD-1 and TIM-3 molecules induced by CD137. Addition of the anti-cancer drug cisplatin to the 2 mAb combination increased overall survival >90 days (and was probably curative) by a mechanism which included a systemic CD8(+) T cell response with tumor specificity and immunological memory. Strikingly, combined treatment of cisplatin and CD137/PD-1 mAb also gave rise to the long-term survival of mice with established TC1 lung tumors. A similar combination of the 2 mAbs and cisplatin should be considered for clinical ‘translation’.
Product Citations
-
Combined prostate cancer vaccine plus immune checkpoint inhibition synergizes to eliminate prostate cancer.
In iScience on 16 January 2026 by Carreno-Galeano, G., Dubey, S., et al.
PubMed
Immunotherapy has improved outcomes in many cancers, yet the clinical benefits remain limited in prostate cancer. We evaluated whether an adenovirus-based bivalent prostate cancer vaccine (Ad-PS2) targeting two tumor antigens could be strengthened by combination with immune checkpoint blockade. Using immunocompetent mouse models, we found that Ad-PS2 combined with low-dose anti-CTLA4 generated robust anti-tumor immunity capable of eliminating established tumors, exceeding the effects of either treatment alone. Tumor-free mice resisted subsequent tumor rechallenge, indicating durable immune protection. Tumor analysis revealed a significant increase in intratumor CD8+ T cell infiltration with Ad-PS2 and anti-CTLA4, whereas anti-PD1 alone produced minimal infiltration and, with the vaccine, provided no therapeutic advantage. These results highlight a mechanistically synergistic interaction between dual antigen-targeted vaccination and CTLA4 blockade and illustrate how rational combination immunotherapy can overcome resistance in prostate cancer. This work defines a strategy that could inform future translational approaches for improving immunologic control of prostate cancer.
-
Potentiating immunotherapy in "immune-cold" solid tumors through orchestrating T cell immunity via tumor-specific genetic engineering.
In Cell Rep Med on 16 December 2025 by He, J., Zhang, C., et al.
PubMed
We engineer a tumor-targeted genetic plasmid vector (PαCD3&LIGHT) to systematically modulate T cell immunity. The tumor-specific telomerase reverse transcriptase (TERT) promoter drives simultaneous expression of tumor necrosis factor superfamily member 14 (LIGHT) and membrane-anchored anti-CD3 single-chain variable fragment (αCD3), which are important immunomodulators with closely clinical relevance. Secreted LIGHT induces high endothelial venule formation and chemokine secretion to recruit circulating lymphocytes, while remodeling extracellular matrix to facilitate immune cell penetration into tumor parenchyma. αCD3 establishes artificial immunological synapses between tumor cells and T lymphocytes. This dual mechanism synergistically establishes tertiary lymphoid structures de novo even within deep tumor regions, harboring stem cell-like CD8+ T cells and driving sustained immunity. Concurrently, αCD3-mediated T cell redirection not only amplifies TCR signaling but also reverses exhausted T cells. The orchestrated T cell immunity significantly potentiates checkpoint inhibitor and chimeric antigen receptor (CAR)-T cell therapies in "immune-cold" tumors without obvious side effects and also remarkably enhances the outcome of human CAR-T cells, demonstrating translational potential in solid tumor immunotherapy.
-
Nodal Expansion, Tumor Infiltration and Exhaustion of Neoepitope-Specific Th Cells After Prophylactic Peptide Vaccination and Anti-CTLA4 Therapy in Mouse Melanoma B16.
In Int J Mol Sci on 4 July 2025 by Shabalkina, A. V., Izosimova, A. V., et al.
PubMed
Peptide vaccines possess several advantages over mRNA vaccines but are generally less effective at inducing antitumor immunity. The bottlenecks limiting peptide vaccine efficacy could be elucidated by tracking and comparing vaccine-induced T-lymphocytes in successful and unsuccessful cases. Here we have applied our recent database of neoantigen-specific T cell receptors (TCRs) to profile tumor-specific T cells following vaccination with a neoantigen peptide vaccine and to correlate this with the response. Mice were vaccinated prophylactically with p30 peptide encoding B16 melanoma neoantigen (K739N mutation in Kif18b gene). The B16F0 melanoma in the vaccinated mice was additionally treated by a CTLA-4 checkpoint blockade. T cells from the tumors, tumor-draining lymph nodes (tdLNs) and vaccine depots were isolated, phenotyped, sorted by subsets and sequenced for TCR repertoires. The vaccine induced the accumulation of tumor-specific CD4+ Th cells in the tdLNs, while in the tumors these cells were present and their frequencies were not changed by the vaccine. These cells also accumulated at the vaccine depots, where they were phenotypically skewed by the vaccine components; however, these effects were minor due to approximately 50-fold lower cell quantities compared to the tdLNs. Only some of the p30-specific Th cells showed tumoricidal activity, as revealed by the reverse correlation of their frequencies in the tdLNs with the tumor size. The CTLA-4 blockade did not affect the tumor growth or the frequencies of tumor-specific cells but did stimulate Th cell motility. Thus, we have shown that tumor-specific Th clones accumulate and/or expand in the tdLNs, which correlates with tumor suppression but only for some of these clones. Tumor infiltration by these clones is not correlated with the growth rate.
-
Mitoxantrone-Encapsulated ZIF-8 Enhances Chemo-Immunotherapy via Amplified Immunogenic Cell Death.
In Adv Sci (Weinh) on 1 April 2025 by Li, J., Lv, W., et al.
PubMed
Chemo-immunotherapy, combining systemic chemotherapeutic drugs and immune checkpoint blockers, is a promising paradigm in cancer treatment. However, challenges such as limited induction of immune responses and systemic immune toxicity have hindered its clinical applications. Here, a zeolite imidazolate framework-8 (ZIF-8) that encapsulates mitoxantrone (MIT), an immune cell death (ICD)-inducing chemotherapeutic agent (MIT@ZIF-8), is synthesized using a one-pot aqueous-phase process. ZIF-8 serves as a dual-functional nanomaterial for chemo-immunotherapy: a carrier to enhance tumor uptake of MIT for improved chemotherapy efficacy, and a pyroptosis inducer to amplify MIT-induced ICD for augmented anti-tumor immune responses. As a result, in vivo administration of MIT@ZIF-8 markedly inhibits tumor growth in both immunologically "hot" colon cancer and immunologically "cold" prostate cancer. Moreover, MIT@ZIF-8 treatment increases the abundance of cytotoxic CD8+ T cells and reduces the amount of immunosuppressive regulatory T cells in tumors, thereby enhancing anti-tumor immunity and sensitizing prostate cancer to anti-CTLA-4 immunotherapy. In summary, MIT@ZIF-8 offers a highly translational approach for chemo-immunotherapy.