InVivoMAb anti-mouse IFNγ
Product Description
Bio X Cell is pleased to offer XMG1.2-CP058. XMG1.2-CP058 is a recombinant, chimeric version of the original XMG1.2 with identical variable domain sequences and constant region sequences converted from Rat IgG1, κ to mouse IgG1, κ for use in murine models. Species-matched chimeric antibodies exhibit regulated effector functions—including Fc receptor binding and complement activation—and cause less immunogenicity and formation of anti-drug antibodies (ADAs) than xenogenic antibodies in animal models. The highly controlled sequence and lack of genetic drift in recombinant antibodies provide more reliable and reproducible results over hybridoma derived antibodies.
Specifications
| Isotype | Rat IgG1, κ |
|---|---|
| Recommended Isotype Control(s) | InVivoMAb rat IgG1 isotype control, anti-horseradish peroxidase |
| Recommended Dilution Buffer | InVivoPure pH 8.0T Dilution Buffer |
| Conjugation | This product is unconjugated. Conjugation is available via our Antibody Conjugation Services. |
| Immunogen | Recombinant mouse IFNγ |
| Reported Applications |
in vivo IFNγ neutralization in vitro IFNγ neutralization ELISPOT Flow cytometry Western blotin vitro Organoids/Organ-on-Chip |
| Formulation |
PBS + 0.01% Tween, pH 8.0 Contains no stabilizers or preservatives |
| Endotoxin |
≤1EU/mg (≤0.001EU/μg) Determined by LAL assay |
| Purity |
≥95% Determined by SDS-PAGE |
| Sterility | 0.2 µm filtration |
| Production | Purified from cell culture supernatant in an animal-free facility |
| Purification | Protein G |
| RRID | AB_1107694 |
| Molecular Weight | 150 kDa |
| Storage | The antibody solution should be stored at the stock concentration at 4°C. Do not freeze. |
| Need a Custom Formulation? | See All Antibody Customization Options |
Application References
-
Takashima S, Sharma R, Chang W, Calafiore M, Fu YY, Jansen SA, Ito T, Egorova A, Kuttiyara J, Arnhold V, Sharrock J, Santosa E, Chaudhary O, Geiger H, Iwasaki H, Liu C, Sun J, Robine N, Mazutis L, Lindemans CA, Hanash AM (2025). "STAT1 regulates immu
PubMed
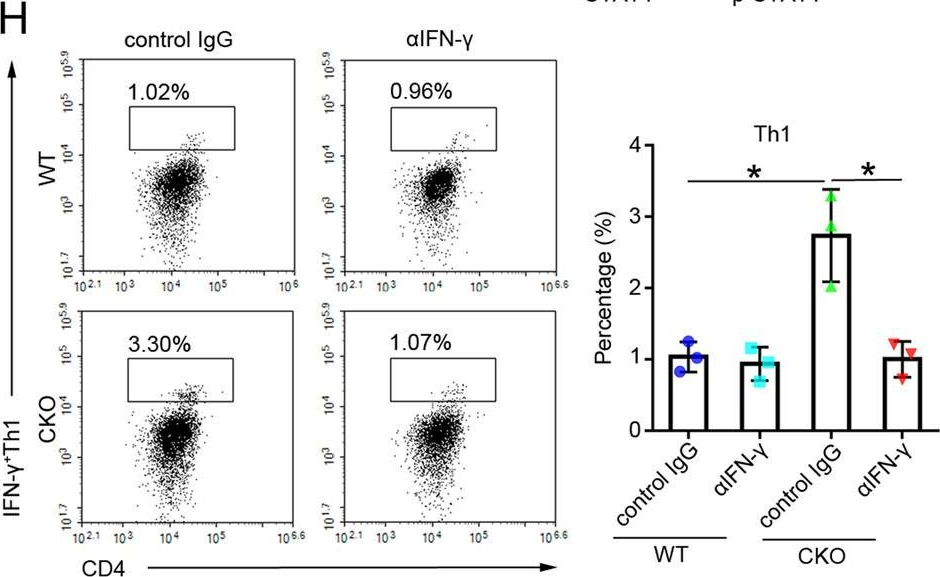
The role of the immune system in regulating tissue stem cells remains poorly understood, as does the relationship between immune-mediated tissue damage and regeneration. Graft vs. host disease (GVHD) occurring after allogeneic bone marrow transplantation (allo-BMT) involves immune-mediated damage to the intestinal epithelium and its stem cell compartment. To assess impacts of T-cell-driven injury on distinct epithelial constituents, we have performed single cell RNA sequencing on intestinal crypts following experimental BMT. Intestinal stem cells (ISCs) from GVHD mice have exhibited global transcriptomic changes associated with a substantial Interferon-γ response and upregulation of STAT1. To determine its role in crypt function, STAT1 has been deleted within murine intestinal epithelium. Following allo-BMT, STAT1 deficiency has resulted in reduced epithelial proliferation and impaired ISC recovery. Similarly, epithelial Interferon-γ receptor deletion has also attenuated proliferation and ISC recovery post-transplant. Investigating the mechanistic basis underlying this epithelial response, ISC STAT1 expression in GVHD has been found to correlate with upregulation of ISC c-Myc. Furthermore, activated T cells have stimulated Interferon-γ-dependent epithelial regeneration in co-cultured organoids, and Interferon-γ has directly induced STAT1-dependent c-Myc expression and ISC proliferation. These findings illustrate immunologic regulation of a core tissue stem cell program after damage and support a role for Interferon-γ as a direct contributor to epithelial regeneration.
-
Takashima S, Sharma R, Chang W, Calafiore M, Fu YY, Jansen SA, Ito T, Egorova A, Kuttiyara J, Arnhold V, Sharrock J, Santosa E, Chaudhary O, Geiger H, Iwasaki H, Liu C, Sun J, Robine N, Mazutis L, Lindemans CA, Hanash AM (2025). "STAT1 regulates immu
PubMed
The role of the immune system in regulating tissue stem cells remains poorly understood, as does the relationship between immune-mediated tissue damage and regeneration. Graft vs. host disease (GVHD) occurring after allogeneic bone marrow transplantation (allo-BMT) involves immune-mediated damage to the intestinal epithelium and its stem cell compartment. To assess impacts of T-cell-driven injury on distinct epithelial constituents, we have performed single cell RNA sequencing on intestinal crypts following experimental BMT. Intestinal stem cells (ISCs) from GVHD mice have exhibited global transcriptomic changes associated with a substantial Interferon-γ response and upregulation of STAT1. To determine its role in crypt function, STAT1 has been deleted within murine intestinal epithelium. Following allo-BMT, STAT1 deficiency has resulted in reduced epithelial proliferation and impaired ISC recovery. Similarly, epithelial Interferon-γ receptor deletion has also attenuated proliferation and ISC recovery post-transplant. Investigating the mechanistic basis underlying this epithelial response, ISC STAT1 expression in GVHD has been found to correlate with upregulation of ISC c-Myc. Furthermore, activated T cells have stimulated Interferon-γ-dependent epithelial regeneration in co-cultured organoids, and Interferon-γ has directly induced STAT1-dependent c-Myc expression and ISC proliferation. These findings illustrate immunologic regulation of a core tissue stem cell program after damage and support a role for Interferon-γ as a direct contributor to epithelial regeneration.
-
Takashima S, Sharma R, Chang W, Calafiore M, Fu YY, Jansen SA, Ito T, Egorova A, Kuttiyara J, Arnhold V, Sharrock J, Santosa E, Chaudhary O, Geiger H, Iwasaki H, Liu C, Sun J, Robine N, Mazutis L, Lindemans CA, Hanash AM (2025). "STAT1 regulates immu
PubMed
The role of the immune system in regulating tissue stem cells remains poorly understood, as does the relationship between immune-mediated tissue damage and regeneration. Graft vs. host disease (GVHD) occurring after allogeneic bone marrow transplantation (allo-BMT) involves immune-mediated damage to the intestinal epithelium and its stem cell compartment. To assess impacts of T-cell-driven injury on distinct epithelial constituents, we have performed single cell RNA sequencing on intestinal crypts following experimental BMT. Intestinal stem cells (ISCs) from GVHD mice have exhibited global transcriptomic changes associated with a substantial Interferon-γ response and upregulation of STAT1. To determine its role in crypt function, STAT1 has been deleted within murine intestinal epithelium. Following allo-BMT, STAT1 deficiency has resulted in reduced epithelial proliferation and impaired ISC recovery. Similarly, epithelial Interferon-γ receptor deletion has also attenuated proliferation and ISC recovery post-transplant. Investigating the mechanistic basis underlying this epithelial response, ISC STAT1 expression in GVHD has been found to correlate with upregulation of ISC c-Myc. Furthermore, activated T cells have stimulated Interferon-γ-dependent epithelial regeneration in co-cultured organoids, and Interferon-γ has directly induced STAT1-dependent c-Myc expression and ISC proliferation. These findings illustrate immunologic regulation of a core tissue stem cell program after damage and support a role for Interferon-γ as a direct contributor to epithelial regeneration.
-
Wang C, Hyams B, Allen NC, Cautivo K, Monahan K, Zhou M, Dahlgren MW, Lizama CO, Matthay M, Wolters P, Molofsky AB, Peng T (2023). "Dysregulated lung stroma drives emphysema exacerbation by potentiating resident lymphocytes to suppress an epithelial
PubMed
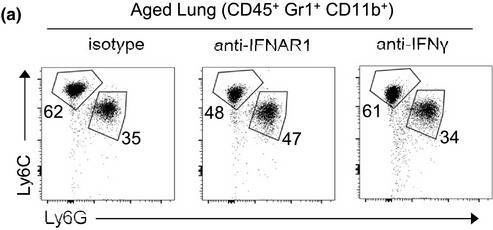
Aberrant tissue-immune interactions are the hallmark of diverse chronic lung diseases. Here, we sought to define these interactions in emphysema, a progressive disease characterized by infectious exacerbations and loss of alveolar epithelium. Single-cell analysis of human emphysema lungs revealed the expansion of tissue-resident lymphocytes (TRLs). Murine studies identified a stromal niche for TRLs that expresses Hhip, a disease-variant gene downregulated in emphysema. Stromal-specific deletion of Hhip induced the topographic expansion of TRLs in the lung that was mediated by a hyperactive hedgehog-IL-7 axis. 3D immune-stem cell organoids and animal models of viral exacerbations demonstrated that expanded TRLs suppressed alveolar stem cell growth through interferon gamma (IFNγ). Finally, we uncovered an IFNγ-sensitive subset of human alveolar stem cells that was preferentially lost in emphysema. Thus, we delineate a stromal-lymphocyte-epithelial stem cell axis in the lung that is modified by a disease-variant gene and confers host susceptibility to emphysema.
Product Citations
-
Intratumoral natural killer cells show reduced effector and cytolytic properties and control the differentiation of effector Th1 cells.
In Oncoimmunology on 6 February 2017 by Paul, S., Kulkarni, N., et al.
PubMed
Natural killer (NK) cells are known to have effector and cytolytic properties to kill virus infected or tumor cells spontaneously. Due to these properties, NK cells have been used as an adoptive cellular therapy to control tumor growth in various clinical trials but have shown limited clinical benefits. This indicates that our knowledge about phenotypic and functional differences in NK cells within the tumor microenvironment and secondary lymphoid tissues is incomplete. In this work, we report that B16F10 cell-induced melanoma recruits the CD11b+CD27+ subset of NK cells at a very early stage during tumor progression. These intratumoral NK cells showed increased expression of CD69, reduced inhibitory receptor KLRG1, and decreased proliferative ability. As compared to splenic NK cells, intratumoral NK cells showed decreased expression of activating receptors NKG2D, Ly49D and Ly49H; increased inhibitory receptors, NKG2A and Ly49A; decreased cytokines IFNγ and GM-CSF; decreased cytokine receptors IL-21R, IL-6Rα, and CD122 expression. Depletion of NK cells led to decrease peripheral as well as intratumoral effector CD4+T-bet+ cells (Th1), and increased tumor growth. Furthermore, purified NK cells showed increased differentiation of Th1 cells in an IFNγ-dependent manner. Anti-NKG2D in the culture promoted differentiation of effector Th1 cells. Collectively, these observations suggest that intratumoral NK cells possess several inhibitory functions that can be partly reversed by signaling through the NKG2D receptor or by cytokine stimulation, which then leads to increased differentiation of effector Th1 cells.
-
Engineered outer membrane vesicles enhance solid tumour CAR-T cell therapy.
In Nat Biomed Eng on 1 April 2026 by Li, X., Li, X., et al.
PubMed
Major challenges facing chimeric antigen receptor (CAR)-T cell therapy for solid tumours include the immunosuppressive tumour microenvironment and the heterogeneity of antigen expression. Bacterial outer membrane vesicles (OMVs) naturally activate the immune system and can be engineered for drug delivery. Here we develop a bacterial OMV-based immunosuppression reversal and optimized antigen decoration platform for CAR-T therapy (BROAD-CAR), in which OMVs are modified to express a high-affinity anti-PD-L1 antibody and load plasmids encoding the target antigen for CARs. By blocking the PD-1/PD-L1 signalling pathway, our tumour-targeting platform enhances the antitumour activity of CAR-T cells both in vitro and in vivo and boosts CAR-T cell expansion by ameliorating the tumour microenvironment. BROAD-CAR also facilitates the in situ antigenic modification of solid tumours and achieves CAR-mediated lysis of antigen-heterogeneous and antigen-negative tumours, inhibiting tumour recurrence and metastasis in the breast cancer mouse models. Our findings highlight a safe and efficient approach to enhance the efficacy and applicability of CAR-T therapy in solid tumours.
-
Metabolically reprogrammed eosinophils impair T cell immunity and cause chronic skin infection.
In EMBO Mol Med on 1 April 2026 by Barinberg, D., Sebald, H., et al.
PubMed
Eosinophils exhibit antimicrobial, cytotoxic and immunoregulatory effects, but our knowledge of their transcriptional and functional heterogeneity is still limited, especially in non-intestinal tissues. Here, we used a mouse model of chronic cutaneous inflammation elicited by the protozoan pathogen Leishmania mexicana to investigate the function and transcriptional dynamics of skin eosinophils. Infection of C57BL/6 mice triggered local and systemic eosinophilia that was driven by type 2 innate lymphoid cells and interleukin-5. Genetic and pharmacological eosinophil depletion led to an enhanced Th1 response, polarization towards M1-like macrophages and resolution of clinical disease, despite an unexpected simultaneous upregulation of IL-4. Single-cell transcriptomics revealed a skin-imprinted trajectory of inflammatory eosinophils that strongly expressed the glucose transporter Slc2a3 (GLUT3) These eosinophils impeded the function of Th1 cells by forming a competitive metabolic niche through preferential glucose uptake. Our findings uncover an inflammatory, metabolically reprogrammed eosinophil population that promotes chronic skin inflammation by limiting protective T cell responses.
-
Lymphodepleting preconditioning impairs host antitumor immunity induced by adoptive T cell therapy in mouse models.
In Nat Commun on 31 March 2026 by Figueroa, D., Vega, J. P., et al.
PubMed
Adoptive T cell therapy (ACT) is effective against hematologic cancers, but the mechanisms underlying durable responses in solid tumors remain unclear. We show that adoptively transferred CD8+ T cells that eradicate established murine tumors promote expansion of host CD8+ T cells exhibiting tumor-reactive and tissue-resident phenotypes that contribute to tumor elimination. Mechanistically, tumor necrosis factor (TNF) from transferred cells induces dendritic cell (DC)-dependent expansion of host CD8+ T cells, conferring protection against ACT-resistant tumor cells lacking the targeted antigen. Lymphodepleting preconditioning promotes expansion of transferred cells and primary tumor eradication but impairs host antitumor immunity and abrogates protection against ACT-resistant tumors. In human tumors, increased TNF/DC/CD8+ T cell profiles correlate with favorable ACT responses and improved survival. These findings reveal a TNF-dependent interplay between transferred and host CD8+ T cells underlying durable antitumor immunity that is impaired by lymphodepleting preconditioning in mouse models, suggesting an underappreciated mechanism of ACT resistance.